Subscribe to be notified when new articles are published. You'll also receive my 2 free ebooks to assist you on your journey. My subscribers also get a treasure trove of info on nutrition, supplements and lifestyle tips on surviving breast cancer. There are moments on...
Read Marnie’s Blog Articles
Titanium Markers in Breast Biopsies: Are They Safe and Do They Stay in the Breast?
Titanium markers are often left in the breast after a biopsy. Are they safe, do they stay, and what should you know? Read this before your biopsy.
Cone Beam Breast Computed Tomography – CBBCT – A More Comfortable and Accurate Alternative to Mammograms
Subscribe to be notified when new articles are published. You'll also receive my 2 free ebooks to assist you on your journey. My subscribers also get a treasure trove of info on nutrition, supplements and lifestyle tips on surviving breast cancer. Mammograms...
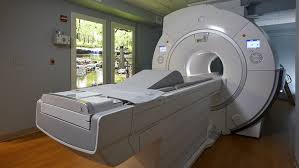
How to Detox After MRI Scans
Subscribe to be notified when new articles are published. You'll also receive my 2 free ebooks to assist you on your journey. My subscribers also get a treasure trove of info on nutrition, supplements and lifestyle tips on surviving breast cancer. In the US alone,...
Why Are We Still Dismissing Soy For Breast Cancer?
One of the questions I most frequently get revolves around whether or not soy should be consumed or avoided for those with estrogen receptor positive (ER+) breast cancer.
The Best Things You Can Do for Lymphatic Health
Subscribe to be notified when new articles are published. You'll also receive my 2 free ebooks to assist you on your journey. My subscribers also get a treasure trove of info on nutrition, supplements and lifestyle tips on surviving breast cancer. Judging from a...
IV Vitamin C and Breast Cancer: What You Need to Know
Subscribe to be notified when new articles are published. You'll also receive my 2 free ebooks to assist you on your journey. My subscribers also get a treasure trove of info on nutrition, supplements and lifestyle tips on surviving breast cancer. IV vitamin C therapy...
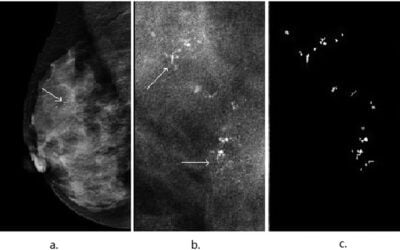
Are Breast Calcifications a Sign of Cancer?
Subscribe to be notified when new articles are published. You'll also receive my 2 free ebooks to assist you on your journey. My subscribers also get a treasure trove of info on nutrition, supplements and lifestyle tips on surviving breast cancer. Are Breast...
Essential Oil Research – Tea Tree Oil
Subscribe to be notified when new articles are published. You'll also receive my 2 free ebooks to assist you on your journey. My subscribers also get a treasure trove of info on nutrition, supplements and lifestyle tips on surviving breast cancer. Essential Oil...
Subscribe For Extra Support
Welcome to the Marnie Clark Breast Care Community. When you join my virtual family you will receive my informative newsletter PLUS my gift to you, these 2 eBooks valued at $47 to empower and support you on your breast cancer journey.
My subscribers also get a treasure trove of info on nutrition, supplements and lifestyle tips on surviving breast cancer.
“Thank you for the email and the meaningful words. I also wanted to thank you for being with me during my treatments. Your emails and posts not only gave me information but lots of courage.” Susan Z, Canada